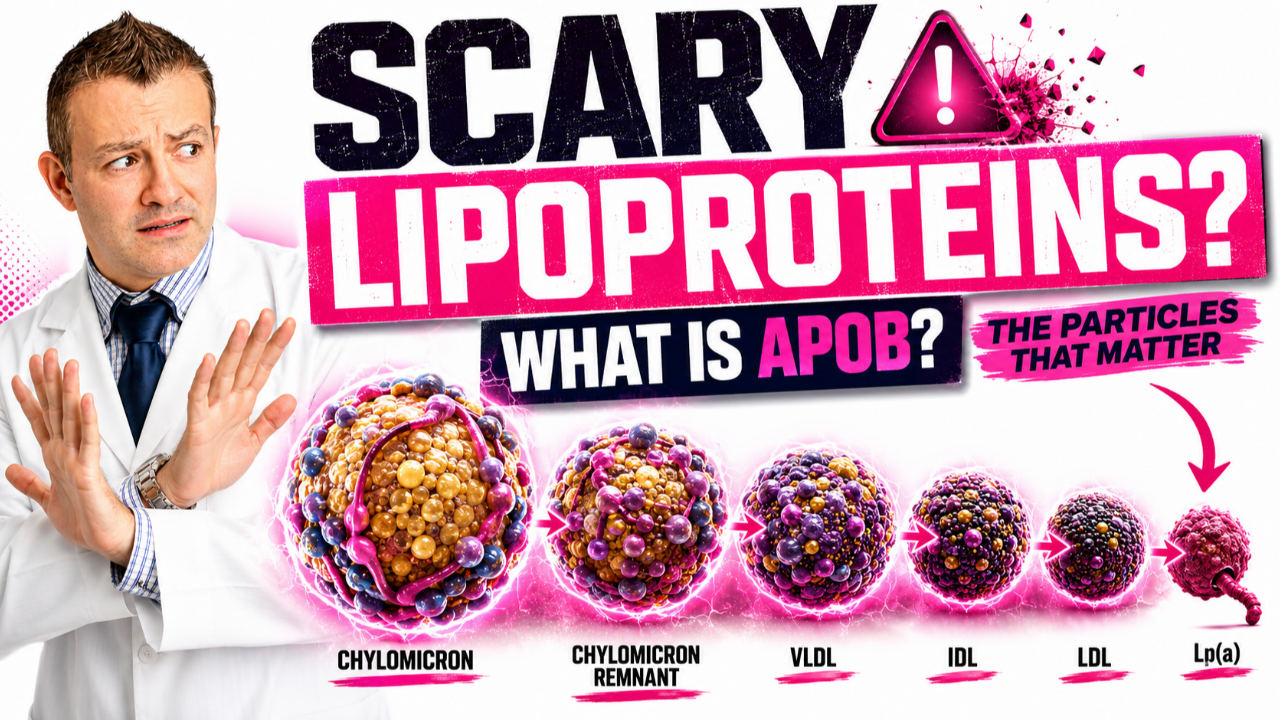
Heart Failure Symptoms: Early Signs, Causes & Treatment
Mar 05, 2026
Understanding Heart Failure: A Guide for Patients
Heart failure is a condition where your heart cannot pump blood as well as it should. Forward flow of blood has decreased. This doesn't mean your heart has stopped working, it means your heart muscle has become weaker or stiffer and can't keep up with your body's needs for oxygen and nutrients.
When your heart isn't pumping effectively, blood can back up in your lungs and other parts of your body, causing fluid to build up. This is why many people with heart failure experience swelling and shortness of breath. Heart failure is a serious condition, but with proper treatment and lifestyle changes, many people live full, active lives.
Types Of Heart Failure: Systolic and Diastolic
Systolic heart failure occurs when your heart muscle becomes weak and cannot squeeze strongly enough to pump blood out to your body, while diastolic heart failure occurs when your heart muscle becomes stiff and cannot relax properly to fill with blood between beats.
In systolic heart failure (also called heart failure with reduced ejection fraction or HFrEF), the heart's pumping power is diminished—typically the heart ejects less than 40% of its blood with each beat, compared to the normal 50-70%.
In diastolic heart failure (also called heart failure with preserved ejection fraction or HFpEF), the heart squeezes normally but the walls have become thick or rigid, so less blood enters the heart before each beat.
Both types lead to similar symptoms, shortness of breath, fatigue, and fluid buildup. In both cases, your body isn't getting enough oxygen-rich blood. Systolic heart failure is more common in men and is often caused by heart attacks or dilated cardiomyopathy, while diastolic heart failure is more common in older adults, women, and people with high blood pressure, obesity, or diabetes.
Treatment differs somewhat between the two: systolic heart failure has several proven medications (ACE inhibitors, beta blockers, SGLT2 inhibitors, and others) that improve survival, while diastolic heart failure has historically been harder to treat, though newer SGLT2 inhibitor medications have recently shown benefit for this type as well.
Heart Failure Infographic Summary:
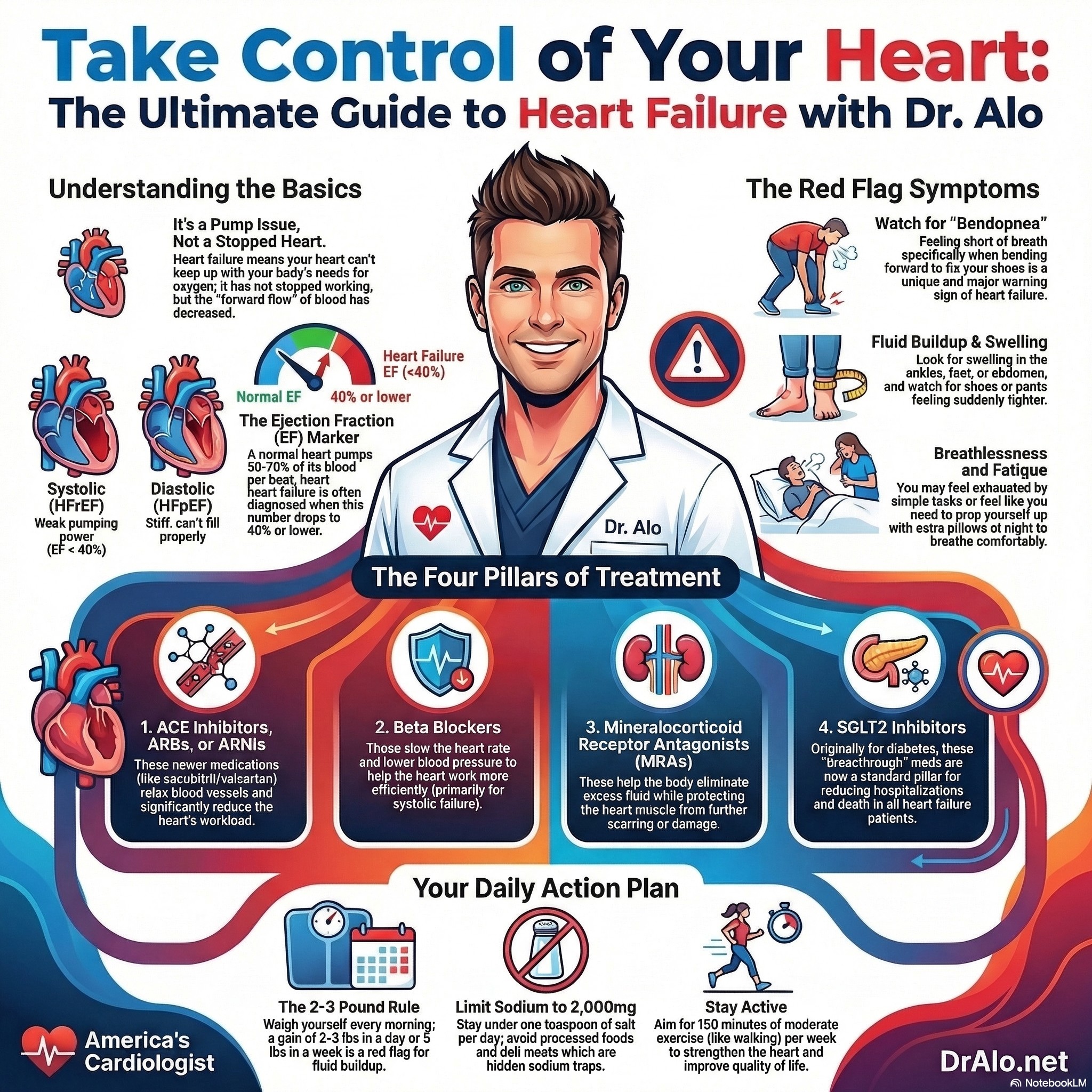
What Are the Symptoms of Heart Failure?
The most common symptoms of heart failure include:
Shortness of breath is often the first symptom people notice. You might feel breathless when climbing stairs, walking, or even lying flat in bed. Some people need to prop themselves up with extra pillows at night to breathe comfortably, or they wake up suddenly feeling like they can't catch their breath.
Swelling typically appears in your ankles, legs, or feet, though it can also occur in your abdomen. You might notice your shoes feel tighter or your pants don't fit the same way. This happens because fluid builds up when your heart can't pump blood effectively through your body.
Fatigue and weakness are very common. You may feel tired all the time and find that activities you used to do easily now leave you exhausted. This happens because your muscles and organs aren't getting enough oxygen-rich blood.
Other symptoms can include a persistent cough (especially when lying down), rapid or irregular heartbeat, wheezing 9often called cardiac wheezing), difficulty concentrating, decreased appetite, and sudden weight gain from fluid retention.
Some people also experience "bendopnea", or shortness of breath when bending forward, such as when tying your shoes. This is a specific sign that suggests heart failure.
What Causes Heart Failure?
Heart failure develops when something damages or weakens your heart muscle. The most common causes include:
High blood pressure is the leading cause of heart failure. When your blood pressure stays high for years, your heart has to work harder to pump blood, which can eventually weaken or stiffen the heart muscle.
Coronary artery disease and heart attacks occur when the arteries that supply blood to your heart become blocked. A heart attack can damage part of your heart muscle, making it harder for your heart to pump effectively. In Western countries, coronary artery disease causes about half of all heart failure cases.
Diabetes significantly increases your risk of developing heart failure, even if you don't have other heart problems. High blood sugar levels over time can damage your heart muscle and blood vessels.
Obesity puts extra strain on your heart and is closely linked to other conditions that cause heart failure, like high blood pressure and diabetes.
Heart valve problems can force your heart to work harder, eventually leading to heart failure. These can be caused by aging, infections, or rheumatic fever.
Inherited heart conditions run in some families. If you have relatives with heart failure or cardiomyopathy (disease of the heart muscle), you may be at higher risk.
Other causes include viral infections of the heart, alcohol or drug abuse (especially cocaine and methamphetamine), certain cancer treatments, thyroid disease, and irregular heart rhythms like atrial fibrillation.
How Is Heart Failure Diagnosed?
It's usually diagnosed on clinical exam. You should be able to know if a patient is in heart failure or not just by talking to them and examining them. However, you will need some testing to figure out which type of heart failure they have.
If your doctor suspects heart failure, you'll undergo several tests:
Blood tests are usually the first step. Your doctor will check for a substance called BNP or NT-proBNP, which your heart releases when it's under stress. Normal levels of these substances make heart failure very unlikely. Your doctor will also check your kidney function, thyroid, blood count, and other important markers.
An electrocardiogram (ECG or EKG) records your heart's electrical activity and can show if you've had a heart attack, have an irregular rhythm, or if your heart is enlarged.
A chest X-ray can show if your heart is enlarged or if there's fluid in your lungs.
An echocardiogram is an ultrasound of your heart and is the most important test for diagnosing heart failure. It shows how well your heart is pumping (measured as "ejection fraction"), the size of your heart chambers, how your valves are working, and whether there are any structural problems. A normal ejection fraction is 50% or higher. If yours is 40% or lower, you have what's called "heart failure with reduced ejection fraction."
Additional tests might include a stress test to see how your heart performs during exercise, or coronary angiography to check for blocked arteries.
Many smartwatches and wearable devices can now detect irregular heart rhythms, which may help your doctor understand what's happening with your heart.
How Is Heart Failure Treated?
Treatment for heart failure has improved dramatically in recent years, and people are living longer, healthier lives than ever before. Your treatment will depend on what caused your heart failure and how severe it is.
Medications
If you have heart failure with reduced ejection fraction (the most common type), your doctor will likely prescribe a combination of four main types of medications, often called the "four pillars" of heart failure treatment:
- ACE inhibitors, ARBs, or ARNIs help relax your blood vessels and reduce the workload on your heart. ARNIs (like sacubitril/valsartan) are newer medications that work even better than older options.
- Beta blockers slow your heart rate and reduce blood pressure, helping your heart work more efficiently. This is not used in diastolic heart failure.
- Mineralocorticoid receptor antagonists (MRAs) help your body get rid of excess fluid and protect your heart from further damage.
- SGLT2 inhibitors were originally developed for diabetes but have been shown to significantly reduce hospitalizations and death in people with heart failure, even if you don't have diabetes.
These four medications work together and are most effective when used in combination. Your doctor will start you on these medications and gradually increase the doses to target levels over several weeks to months.
Other medications you might need include:
- Diuretics (water pills) help reduce fluid buildup and relieve swelling and shortness of breath. You may need to adjust your dose based on your daily weight.
- Additional medications like digoxin, ivabradine, or vericiguat may be added if you continue to have symptoms despite the four main medications.
Devices
Some people with heart failure benefit from implanted devices:
- Pacemakers or defibrillators can help regulate your heart rhythm and protect against dangerous irregular heartbeats.
- Cardiac resynchronization therapy (CRT) uses a special pacemaker to help both sides of your heart pump together more efficiently.
Advanced Therapies
For people with very severe heart failure that doesn't improve with medications, options include:
- Ventricular assist devices (VADs), which are mechanical pumps that help your heart pump blood
- Heart transplantation for eligible patients
- Iron Replacement
Many people with heart failure have iron deficiency, which can make fatigue worse. If blood tests show you're iron deficient, intravenous iron replacement can improve your energy levels and quality of life.
Lifestyle Changes That Help
Medications are essential, but lifestyle changes are equally important for managing heart failure:
Monitor your weight daily. Weigh yourself every morning after using the bathroom but before eating breakfast. A sudden weight gain of 2-3 pounds in a day or 5 pounds in a week can mean fluid is building up. Call your doctor if this happens—you may need to adjust your water pill.
Limit salt (sodium). Too much salt causes your body to retain fluid, which makes heart failure worse. Aim for less than 2,000 mg of sodium per day. Avoid processed foods, canned soups, deli meats, and restaurant meals, which are often very high in sodium. One teaspoon of salt contains 2,000 mg of sodium.
Watch your fluid intake. Your doctor may recommend limiting how much you drink each day, typically to about 2 liters (8 cups). This includes all liquids—water, coffee, tea, soup, and even ice cream.
Exercise regularly. This might seem counterintuitive, but regular physical activity actually helps strengthen your heart and improves your symptoms. Aim for at least 150 minutes of moderate exercise per week, such as walking. Start slowly and gradually increase your activity level. Cardiac rehabilitation programs provide supervised exercise and education specifically designed for people with heart failure.
Maintain a healthy weight. If you're overweight, losing weight can significantly reduce the strain on your heart. If you're underweight or losing weight unintentionally, tell your doctor, as this can be a sign of worsening heart failure.
Eat a heart-healthy diet. Focus on whole grains, fruits, vegetables, lean proteins, and healthy fats. The Mediterranean diet and plant-based diets have shown particular benefits for heart health.
Quit smoking and limit alcohol. Smoking damages your heart and blood vessels. Alcohol can weaken your heart muscle and should be limited or avoided completely.
Manage stress. Chronic stress can worsen heart failure. Consider relaxation techniques, meditation, yoga, or counseling to help manage stress and anxiety.
Get vaccinated. Get your annual flu shot and pneumonia vaccine to prevent infections that could worsen your heart failure.
Take your medications exactly as prescribed. Don't skip doses or stop taking medications without talking to your doctor first, even if you feel better.
Living With Heart Failure
Heart failure is a chronic condition that requires ongoing management, but many people live well with it for years. Here are some important tips:
Know the warning signs that your condition is getting worse:
- Sudden weight gain
- Increased swelling in your legs, ankles, or abdomen
- Increased shortness of breath, especially when lying down
- Waking up at night unable to breathe
- Persistent cough or wheezing
- Extreme fatigue or weakness
- Decreased appetite or nausea
- Confusion or difficulty thinking clearly
- Rapid or irregular heartbeat
If you experience any of these symptoms, contact your doctor right away. Don't wait to see if they get better on their own.
Attend all your medical appointments. Regular follow-up visits allow your doctor to monitor your condition, adjust medications, and catch problems early.
Consider cardiac rehabilitation. These programs provide supervised exercise, education about heart failure, nutritional counseling, and emotional support. They can significantly improve your quality of life and help you manage your condition more effectively.
Build a support system. Living with heart failure can be challenging emotionally. Don't hesitate to ask for help from family, friends, or support groups. Many people with heart failure also experience depression or anxiety, which are treatable conditions—talk to your doctor if you're struggling emotionally.
Plan ahead. As your condition progresses, it's important to discuss your goals and preferences for care with your doctor and loved ones. This includes thinking about advanced therapies, quality of life, and end-of-life wishes.
Heart Failure Bottom Line
Heart failure is a serious condition, but it's also very treatable. With the right combination of medications, lifestyle changes, and medical care, many people with heart failure live full, active lives. The key is working closely with your healthcare team, taking your medications as prescribed, monitoring your symptoms, and making healthy lifestyle choices.
Remember that heart failure treatment has improved dramatically in recent years. New medications and therapies continue to emerge, offering hope for even better outcomes in the future. By taking an active role in your care and following your treatment plan, you can manage your symptoms, stay out of the hospital, and enjoy a good quality of life.
References:
Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure. Circulation. 2022;145(18):e895-e1032. https://www.ahajournals.org/doi/10.1161/CIR.0000000000001063
McDonagh TA, Metra M, Adamo M, et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. European Heart Journal. 2021;42(36):3599-3726. https://academic.oup.com/eurheartj/article/42/36/3599/6358045
McMurray JJV, Packer M, Desai AS, et al. Angiotensin–Neprilysin Inhibition versus Enalapril in Heart Failure (PARADIGM-HF). New England Journal of Medicine. 2014;371(11):993-1004. https://www.nejm.org/doi/full/10.1056/NEJMoa1409077
McMurray JJV, Solomon SD, Inzucchi SE, et al. Dapagliflozin in Patients with Heart Failure and Reduced Ejection Fraction (DAPA-HF). New England Journal of Medicine. 2019;381(21):1995-2008. https://www.nejm.org/doi/full/10.1056/NEJMoa1911303
Packer M, Anker SD, Butler J, et al. Cardiovascular and Renal Outcomes with Empagliflozin in Heart Failure (EMPEROR-Reduced). New England Journal of Medicine. 2020;383(15):1413-1424. https://www.nejm.org/doi/full/10.1056/NEJMoa2022190
Anker SD, Butler J, Filippatos G, et al. Empagliflozin in Heart Failure with a Preserved Ejection Fraction (EMPEROR-Preserved). New England Journal of Medicine. 2021;385(16):1451-1461. https://www.nejm.org/doi/full/10.1056/NEJMoa2107038
Taylor RS, Walker S, Smart NA, et al. Impact of Exercise Rehabilitation on Exercise Capacity and Quality-of-Life in Heart Failure: Individual Participant Meta-Analysis. Journal of the American College of Cardiology. 2019;73(12):1430-1443. https://pubmed.ncbi.nlm.nih.gov/30922474
Anker SD, Comin Colet J, Filippatos G, et al. Ferric Carboxymaltose in Patients with Heart Failure and Iron Deficiency (FAIR-HF). New England Journal of Medicine. 2009;361(25):2436-2448. https://www.nejm.org/doi/full/10.1056/NEJMoa0908355
Thibodeau JT, Turer AT, Gualano SK, et al. Characterization of a novel symptom of advanced heart failure: bendopnea. JACC Heart Failure. 2014;2(1):24-31. https://pubmed.ncbi.nlm.nih.gov/24622115
O'Connor CM, Whellan DJ, Lee KL, et al. Efficacy and Safety of Exercise Training in Patients With Chronic Heart Failure (HF-ACTION). JAMA. 2009;301(14):1439-1450. https://jamanetwork.com/journals/jama/fullarticle/183710
Yancy CW, Jessup M, Bozkurt B, et al. 2017 ACC/AHA/HFSA Focused Update of the 2013 ACCF/AHA Guideline for the Management of Heart Failure. Circulation. 2017;136(6):e137-e161. https://www.ahajournals.org/doi/10.1161/CIR.0000000000000509
Ponikowski P, Voors AA, Anker SD, et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. European Heart Journal. 2016;37(27):2129-2200. https://academic.oup.com/eurheartj/article/37/27/2129/1748921
Still Have Questions? Stop Googling and Ask Dr. Alo.
You’ve read the science, but applying it to your own life can be confusing. I created the Dr. Alo VIP Private Community to be a sanctuary away from social media noise.
Inside, you get:
-
Direct Access: I answer member questions personally 24/7/365.
-
Weekly Live Streams: Deep dives into your specific health challenges.
-
Vetted Science: No fads, just evidence-based cardiology and weight loss.
Don't leave your heart health to chance. Get the guidance you deserve. All this for less than 0.01% the cost of health insurance! You can cancel at anytime!
[👉 Join the Dr. Alo VIP Community Today]